Eve Health’s Gynaecologists perform Mirena insertion procedures at our Women’s Health Clinic in Brisbane . Read more about the procedure below or get in touch with our friendly reception staff on 07 3332 1999 to book a consultation.
What is a Mirena Insertion Used For?
Mirena is a long acting, reversible hormone releasing contraceptive device that is inserted into the womb, i.e. an intrauterine contraceptive device (IUCD) and sits in the uterus like a copper IUD. It can be used as a contraceptive agent or to control heavy periods. IUCDs are suitable for women regardless of whether they have had a baby, and are also suitable for teenagers.
How does Mirena work?
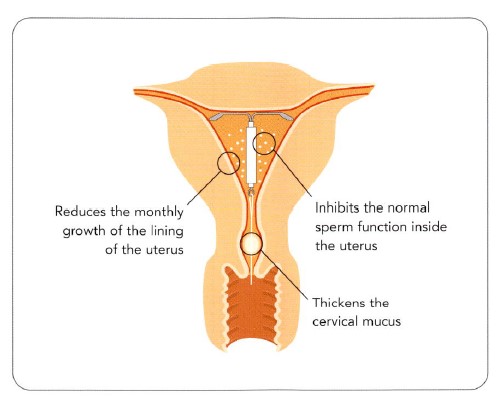
Mirena is a thin plastic T-shaped device containing a synthetic female hormone, known as levonorgestrel, a progesterone. Progesterone is a contraceptive agent found in other preparations, such as “the pill”. This hormone thickens the mucous in the cervix, trapping sperm and reduces the monthly growth of the lining of the womb (endometrium). It does not routinely suppress ovulation.
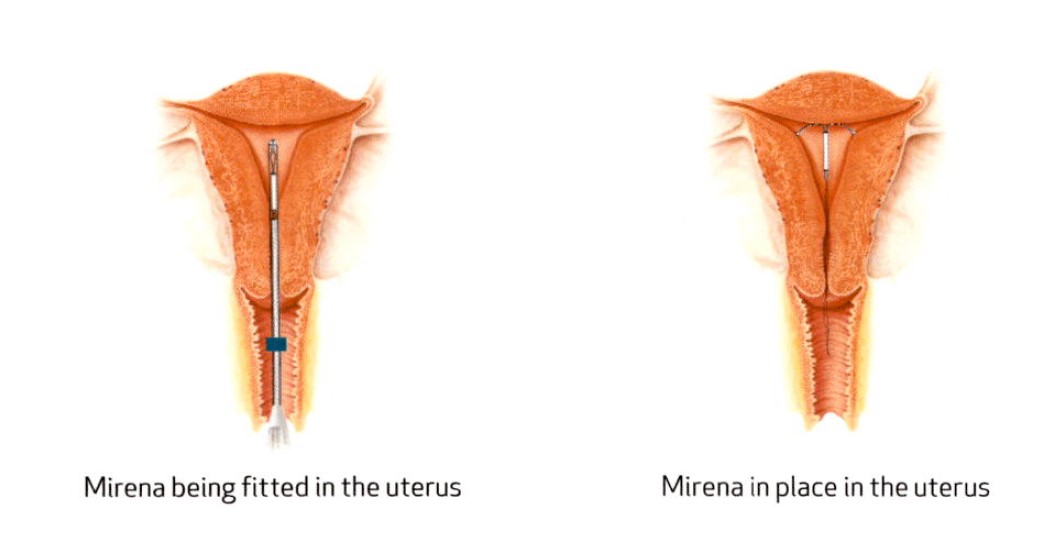
How is this inserted?
The Mirena insertion procedure is performed in our Brisbane CBD consulting rooms by your Gynaecologist. Anaesthesia is not normally required. The Mirena is inserted in a process similar to the taking of a Pap smear, but the passage of the Mirena into the uterus often causes some period-like cramps. The procedure itself takes approximately 15 minutes. Sometimes, the Mirena is inserted at the time of another procedure, such as a hysteroscopy. Following insertion, you will not be able to feel the device, but you should be able to feel the threads of the device with your fingers. The device is removed in a procedure similar to the insertion.
We recommend that you take some simple analgesia such as two ibuprofen and two paracetamol 20 minutes before hand and arrange for someone to drive you home from our Brisbane rooms afterwards. Most women tolerate the procedure well and are fine to attend work or school the following day.
How long does Mirena last?
The device stays in the uterus and remains effective for a maximum of five years, but may be removed sooner if desired. Fertility returns soon after removal. The device does not dissolve and must be removed.
How effective is Mirena? / Can You Get Pregnant On Mirena?
Mirena is extremely effective in the prevention of pregnancy and protective from the time of insertion, provided it is inserted at the right time of your cycle. If more than 1000 women use Mirena for one year, not more than two of them will fall pregnant. It does not require any input from you after insertion and is not generally affected by illness. However, no contraceptive method is one hundred percent reliable.
Does Mirena stop periods?
Mirena has the advantage of making periods very light or non-existent for up to 90% of women.
What are the disadvantages of Mirena?
It does not prevent sexually transmitted diseases. It must be removed upon completion. It can cause light, unpredictable bleeding and irregularities of your menstrual cycle, particularly in the first three months after insertion. The Mirena can cause some cramping, but this usually dissipates within the first few days of insertion. It can have some mild hormonal side effects in sensitive women. Only 1/10th of the progesterone dose can be measured in the blood, so blood hormone levels are very low. The risk of infection is very low for IUCDs, less than 1 in 1000. Your doctor may test for any STIs before insertion of the IUCD to ensure the risk remains low.
When should Mirena be inserted?
Mirena is ideally inserted just after completion of the period but can be anytime in the cycle.
What are the Possible Risks of this Mirena?
Every contraceptive method has associated risks and side-effects. Complications include, but are not limited to:
At the time of insertion
Discomfort at the time of and immediately after insertion; introduction of infection; perforation of the uterus.
Menstrual control
You can expect some change in your periods – the exact effect is difficult to predict; most women will stop having periods, and in the remainder periods become lighter or less regular; however, most women will experience spotting in the first six months after insertion and this may be troublesome.
Expulsion
Rarely, the device may be expelled during the menstrual period; therefore, you should check for the threads of the device after each period or about once a month.
Other effects
A number of other side effects have been reported, including headaches, breast tenderness, and changes in libido; most of these are self limiting. Occasionally, the threads may be felt by your partner, and if this causes discomfort, these can be adjusted. Sometimes the threads become looped up inside the uterus making it more difficult to remove.
Any other specific risks and complications will be discussed prior to the procedure.
What if I have any problems?
You should seek medical attention if you experience:
- Fever or feeling unwell
- Offensive discharge or heavy bleeding
- Intractable nausea or vomiting
- Severe pain
- Inability to feel the threads inside the vagina
Please contact our Brisbane clinic on 07 3332 1999 or attend your nearest hospital emergency department if you require urgent attention.
Information booklets
These information booklets have been put together by Bayer Australia, the manufacturer of Mirena & Kyleena. We have also made a Mirena pre-insertion and post-insertion guides available for download. Please note that other than the Kyleena having a slimmer profile, there is no difference in the process of inserting or removing either a Mirena or Kyleena. Our gynaecologists have paper copies of these booklets available for you to take home after your consult with us, but feel free to download these to improve your knowledge prior to your appointment:
Eve Health also offer a range of other contraception options to Brisbane women – learn more here.
Meet Our Local Brisbane Gynaecologists
How to Book A Mirena Insertion Procedure in Brisbane.
Our Gynaecologists conduct Mirena Insertion procedures at both our our Brisbane locations – find us at:
- 55 Little Edward Street, Level 1 Boundary Court, Spring Hill, Brisbane 4000 &
- Brookwater Specialist Suites, Mater Health Centre, 2 Tournament Drive, Brookwater QLD 4300
Call us now on 07 3332 1999 or click on ‘Book Online Now’ at the top of this page to book a Mirena insertion procedure at one of our Brisbane locations.
Comments are closed.